New Ugandan rules allow HIV care during lockdown
Kikonyogo Kivumbi is the executive director of the Uganda Health…
LGBTI and health rights activists in Uganda have welcomed new guidance from Uganda’s Ministry of Health about continued uninterrupted access to anti-HIV medications, tuberculosis treatments and management of sexually transmitted infections (STIs) during the current countrywide Covid-19 lockdown.
From the African Human Rights Media Network
By Kikonyogo Kivumbi
Uganda’s Ministry of Health has issued guidelines about how vital HIV/AIDS services can continue with minimal disruption during the current 14-day countrywide Covid-19 lockdown.

The guidelines, covering a wide range of health services, were developed by the ministry in consultation with civil society groups in the fight against the HIV pandemic.
Among dozens of specific guidelines, the announcement calls for the establishment of new Community Drug Distribution Points (CDDPs) that will allow people to get their medications without extensive travel.
They also call for regional and local cooperation to ensure that critical HIV services are not interrupted during the Covid-19 lockdown.
The ministry’s announcement came after an outcry from many Ugandans that the lockdown, announced March 30, stops them from getting medical refills, including anti-retroviral (ART) anti-HIV medication. The lockdown bans public transport and private cars in order to limit the spread of the Covid-19 virus.
These are the guidelines:
UGANDA MINISTRY OF HEALTH COVID-19 INFECTION PREVENTION AND CONTROL GUIDANCE FOR HIV SERVICES DELIVERY
This guidance will continue to be updated as new guidance on Covid-19 evolves globally.
The Ministry of Health [MoH] emphasizes the importance of maintaining critical HIV prevention, care and treatment services during Covid-19 to reduce vulnerability of PLHIV [people living with HIV] to Covid-19, ensure continuity of ART therapy and accelerated decongestion of health facilities to minimize transmission of Covid-19.
General considerations
District Teams (Supported by the Regional Implementing Partner)
- The district will maintain its role in leading the implementation of all comprehensive HIV services.
- The regional Implementation Partners will work with the districts to ensure that critical HIV services are not interrupted during the Covid-19 response period. They will provide the necessary technical and financial support.
- District health officers and ART clinic in charges will ensure that skeletal staff is available at facilities to: attend to the clients seeking HIV and TB services in the ART clinics; record details of clients served; quantify ARVs and other drug supplies; and place emergency orders.
- The districts with support from the IP should adopt the use of telephones and internet platforms to communicate to facilities and other stakeholders, including conduct trainings and mentorships.
- The districts with support from the IP will work with the existing Networks of People living with HIV to ensure the uninterrupted supply of ART to all recipients of care.
Networks of PLHIV and Civil society
- The PLHIV networks at national level will continue working with MoH, through the national task force, to coordinate the national HIV response to ensure safety of clients and uninterrupted supply of ARVs.
- The PLHIV networks at the district level will work with districts, through district task force, to monitor coordination and provide timely feedback on the quality of services during the response.
- The peer support staff at HIV service points (such as YAPs, Linkage facilitators, peer/mentor mother) should have their services at the facility suspended until the Covid-19 pandemic is under control. The PLHIV peers may work from home using phones to follow-up clients: remind them of appointments, drug pickups and linkage to nearest community ART services points.

Health facilities
The facilities will display toll-free and other telephone numbers for Covid-19 response teams in visible places so that clients can save them in their phones or write them down.
- All ART, TB and other HIV related clinics should have functional safe thermometers.
- All clients who come to the clinic must have their temperature taken.
- Use telephone calls, SMS, social media platforms to communicate to clients and other stakeholders on services availability, follow up, adherence support and clinic attendance among others.
- Health Providers will use the appropriate Personal Protective Equipment (PPE) for all staff. If a Client is suspected to have Covid-19, a gown and goggles should be used in addition to gloves and medical face mask (where feasible). Face mask and gloves are most important PPE.
- ART Providers and Clients should practice frequent hand hygiene, including before and after patient care, when coming into contact with secretions, before eating and after using the toilet.
- Maintain infection prevention standards in the ART clinic by sanitizing all surfaces e.g. with hypochlorite per MOH guidelines.
- Inform MOH, relevant authorities of any suspected Covid-19 case among the ART patients. Documenting the clinical course of Covid-19 in PLHIV is important to inform optimal care.
- Monitor the number of HIV and TB service providers that are tasked to work on Covid-19.
- Ensure continuous antiretroviral therapy (ART) provision to current recipients of care based on the available stocks of ARVs at the site in order to maintain virologic suppression.
- Health facilities should accurately document the contact details of the clients who come to seek health services for easier follow up in case of Covid-19 exposure.
- Conduct on a regular basis ongoing activities of Information, education and communication (IEC) for the recipients of care to learn about the signs and symptoms of Covid-19 using hand-out messages, telephone calls/SMS, social media platforms and mass media.

Triage
- Facilities must take temperature measurements for all PLHIV clients on arrival at the clinic.
- Patients presenting with fever, cough, flu like/ respiratory symptoms) should be isolated immediately and infection prevention and control observed.
- Screen for TB using the ICF guide at all entry points.
Community activities
The general community health services including HIV testing, HIV Prevention services and TB activities are temporarily stopped as per the Presidential directive on community gatherings.
Supply chain considerations
Facilities with inadequate stocks should place emergency orders for ARVS. However, all facilities must ensure that sufficient stocks of drugs regimens are available during this time. Districts and partners should support inter-facility and inter-district commodity transfers, where applicable.
HIV prevention services
For HIV prevention, most services are community based and require mobilization using community gatherings, and or interaction with several community members. This poses a risk of exposure and transmission of the virus to the community and services providers who are mostly lay persons. Its therefore recommended that all community activities including mobilization, outreaches, meetings and workshops are temporarily put on hold.
HIV testing services [HTS]
- During this interim period, all community activities including HTS outreaches are suspended.
- Facility-based HTS should continue in: Testing in ANC, labor/maternity, early infant diagnosis (EID), in-patient department for diagnostic testing, people with TB, STIs, and
malnutrition, Assisted Partner Notification, and index client testing. - Use of self-testing outside of the clinic setting should be encouraged.
Safe male circumcision [SMC]
- The community camps including community mobilization are suspended. The SMC services shall be offered as a routine service in facility on appointment to avoid crowding.
- The health workers offering SMC must ensure that waiting time for clients is reduced and, at any one time, not more than ten (10) clients should be waiting for the service.
- The Post-operative follow-up for clients already circumcised should continue using telephone calls and clinic visit for clients with adverse events
Safe spaces
- AGYW ( Adolscent Girls and Young Women) safe spaces are temporally closed as per the presidential directive.
- The facility should focus on line listing clients.
- The AGYW should continue accessing the non-curriculum-based services at the health facilities.
- At DICs walk in services will be provided but no more than 10 individuals should be served at any one time.
- Social gathering at DIC [drug information centre] must stop in line with the Presidential directive on social distancing
- KPs [key populations most at risk], AGYWs and services providers are encouraged to use social media platforms for communication.
Continuity of PrEP services [pre-exposure prophylaxis — medication taken daily to prevent HIV].
- Facilities should evaluate the stock medicines available at their sites
- Where stocks allow, individuals already on PrEP should be given a 3-month drug supply.
- When possible, follow up and adherence support of clients on PrEP should be done using telephone, SMS, social media platforms.
HIV treatment services including PMTCT [Prevention of mother-to-child transmission] services
These guidelines are aimed at reducing crowding of clients at ART delivery points as well as ensuring continued access to ART during the COVID-19 pandemic., ART delivery is majorly facility based which may potentially increase risk of the spread of the virus within the
facility, therefore, focus should be placed on decongesting the facilities.
Multi-month dispensing (MMD)
- Multi-month dispensing (MMD) of three to six months is recommended for all clients regardless of age and viral load. This however should be based on availability of adequate ARV stock across the different drug regimens at the facility.
- The Facility should systematically call all clients with scheduled clinic visit in the next month for their ART refills and viral load testing if due.
- The facility should deliver ARVs to the nearest community point for clients who are not able to come to the facility. This can be through quick establishment of CDDPs [Community Drug Distribution Points].
Community drug distribution
- Clients receiving their care and refills through Community Drug Distribution Points (CDDPs) and Community Client Led ART Delivery (CCLADs) should continue receiving their care and refills through the same approaches.
- Infection Prevention and Control (IPC) measures should be emphasized at all times.
- Facilities should support clients to form CCLADs as a measure of decongesting the facility-based ART service delivery points.
- The following categories of clients should be maintained on monthly appointments
and refills at the facility. Howwever IPC measures should be adhered to.
– Virally nonsuppressed
– Newly initiated on ART
– The very sick e.g. clients co-infected with TB and are in intensive phase of TB treatment
– Pregnant mothers
– Lactating mothers with babies below 6 months of age - Facilities should suspend all Facility Based Groups (FBGs) such as the family support groups, Adolescent groups, teen clubs etc. until further notice. Members of such groups should be given multi-month refills if they qualify or else monthly appointments and refills with proper scheduling to avoid congestion at the ART service delivery points.
TB/HIV Services
The majority of clients in the HIV and TB clinic present with cough and other symptoms that may simulate the presenting signs and symptoms of Covid-19. This presents a challenge of screening for Covid-19. Clients who have Covid-19 may be mis-diagnosed.
- With PPE [personal protective equipment] in place, the usual recommended screening for TB should continue and in addition take off recommended samples for Covid-19 testing from suspects (see MOH leaflet for samples to be taken).
- ART refills and anti-TB/TPT refills should be aligned for all PLHIV co-infected with TB or on TB preventive treatment.
- Not all cough is Covid-19, TB screening should be conducted but IPC measures should be adhered to.
- Ensure that all presumptive cases receive TB diagnostic test, Initiate TB treatment for positive ones.
- Coughing patients should be advised to practice home based self-isolation and referral of “suspects” should continue while being investigated for both diseases while waiting for result.
- Meanwhile if TB is confirmed, TB treatment should not be delayed while waiting for the corona test result. Having two comorbidities can worsen the client’s outcome more especially now that there is no treatment for Covid-19.
- Supportive treatment should continue for those who are negative for TB and negative for Covid-19 as outlined in the Uganda guidelines for management of upper or lower respiratory disease.
- TPT/IPT [TB Preventive Treatment, especially for people living with HIV, including anti-TB isoniazid preventive therapy or IPT) drugs should be provided for 6 months and patients monitored through phone calls
TB treatment
- Ensure alignment to HIV DSDM [Differentiated Service Delivery Models, used for determining the appropriate medical care for patients with both TB and HIV infections]
- Dispense TB medicines for 2 months for newly diagnosed patients
- Dispense amount of TB medicines to complete the remaining period of the intensive phase for TB patients who are already in care.
- Dispense up to 2 months of drug refill for patients in the continuation phase
- Drugs may be dispensed to patients at any nearby TB diagnostic and treatment facility
MDR-TB [multi-drug-resistant tuberculosis]
- Inpatients should stay on the ward for their DOT [direct observation of therapy]
- For patients under care at follow up facilities, health workers shall deliver medicine/treatment support at follow up facilities
- Treatment support should be identified to observe DOT at home and report any issues to the health worker promptly.
- A supply of MDR-TB drugs of up to 2months should be offered to the patient and treatment supporter where it is available
- Patients will access monthly reviews as soon as the situation allows





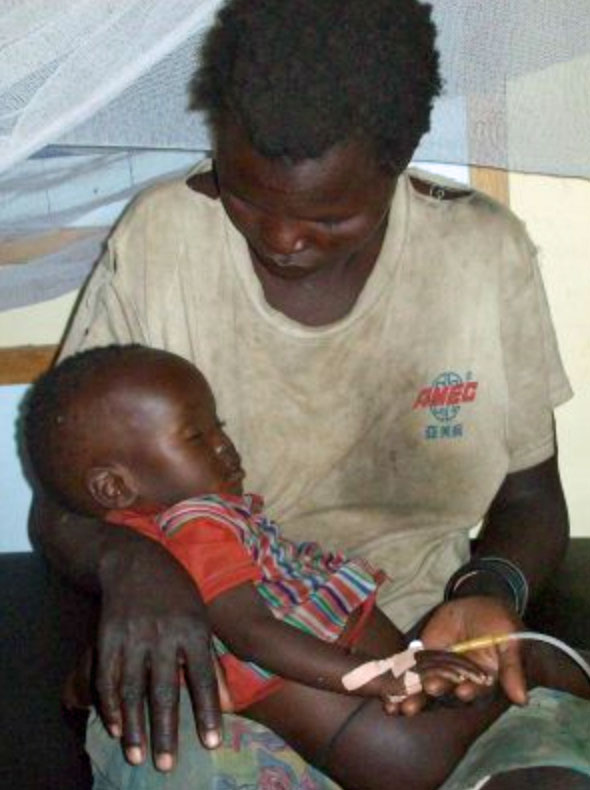
In retrospect would it have been a good idea to give this mother notice of the pending photograph to allow her the human dignity of being able to prepare for the camera? In placing her best foot forward she may have wanted to portray herself and her baby in a different light.
Kikonyogo Kivumi responds:
You’re right, James. That’s what everyone would want. The only difference here is human rights defenders work with communities in extreme vulnerabilities to bring their lived realities to boardrooms. Human rights defenders live and tell the realities they see. When we talk of mothers losing their babies to preventable, curable or manageable diseases in Sub-Saharan Africa because politicians have stolen taxpayers’ money. This and so many scenes is what makes us take the risk and get to frontlines to promote human dignity. The newsworthiness of this picture is overwhelming.